Training Didn’t Help
 My name is Dr. Peter Megdal, and this is my story of curing heart disease. In 2010 I noticed a steep drop in my power output during races. Racing cyclists have power meters that are attached to our bikes so we can accurately measure how strong we are in training and competitions. I was 50 years old, and my coach and my friends all told me that this was because I was getting older, but I knew a 15% drop was pretty steep and not normal especially in just one or two years.
My name is Dr. Peter Megdal, and this is my story of curing heart disease. In 2010 I noticed a steep drop in my power output during races. Racing cyclists have power meters that are attached to our bikes so we can accurately measure how strong we are in training and competitions. I was 50 years old, and my coach and my friends all told me that this was because I was getting older, but I knew a 15% drop was pretty steep and not normal especially in just one or two years.
For the next four years, I trained harder and differently, but saw no improvement in my performance and got concerned and curious, so I sought medical advice. I looked for the best doctor in the area which happened to be a cardiologist at Mass General Hospital who specialized in athletes. He suggested that I try a maximum oxygen uptake stress test which is not done generally for people that have suspected heart disease, but he thought it would be good since I was a high-level athlete.
Here Come The Tests
 In 2013, the year before, I got third at the regional cycling time trial championships in my age group. After getting tested, my oxygen consumption was so high my doctor thought that everything was okay even though I had a signal on my EKG that showed an ST segment depression that had a horizontal characteristic to it. This indicates cardiac ischemia or reduced blood flow to the heart. My doctor believed that this was an artifact and that the only way to ensure that I had no disease was to undergo an angiogram (where they stick a wire in your artery with a dye to inject and view with an x-ray to take an image of the heart arteries) which is the golden standard to see if there are actually blockages in the arteries restricting blood flow.
In 2013, the year before, I got third at the regional cycling time trial championships in my age group. After getting tested, my oxygen consumption was so high my doctor thought that everything was okay even though I had a signal on my EKG that showed an ST segment depression that had a horizontal characteristic to it. This indicates cardiac ischemia or reduced blood flow to the heart. My doctor believed that this was an artifact and that the only way to ensure that I had no disease was to undergo an angiogram (where they stick a wire in your artery with a dye to inject and view with an x-ray to take an image of the heart arteries) which is the golden standard to see if there are actually blockages in the arteries restricting blood flow.
I underwent the test which showed that I had five significant blocks in several of the arteries including the left anterior descending (LAD), the right coronary artery (RCA) and two branches off of the LAD or left anterior descending artery, the largest being 70% in my right coronary artery. Consenting to a stent, I believed that this would fix my problem. I felt fine after and began riding my bike only about three days after the procedure. It was the fall of 2014 and the offseason for racing, but I continued to train hard. One of the reasons I worked so hard was I knew I was undergoing another exercise test in December and wanted to have a good outcome.
Research Brought Me To The Facts
However, it turned out that my oxygen uptake dropped another 5 or so percent and of course this is very disappointing to me. About the same time, I started reading significant literature on how to reverse heart disease including the book from Caldwell Esselstyn, “Reversing Heart Disease.” I also began reading “The China Study” by Colin Campbell. Because of my doctoral training, I understood that you couldn’t believe everything you read particularly in the popular literature.
I began researching the original studies to see if there is a factual basis to the books -in other words, were the books accurate. What I found shocked me … it seemed that a low-fat, whole food plant-based diet eliminating all added fats and eating no animal products seem to be the way to go. It took me about five months of adjusting my attitude to actually take this all in simply because I love eating meat, drinking milk, and so forth. After all, I grew up in Texas, and everyone pretty much had a cow in their backyards.
A New Diet Led To A New Life
 So in March of 2015, I made the personal decision and so did my wife to not eat any meat. Since I knew this was the right thing to do but without really preparing for it, I was really hungry for about 2 weeks. I then started figuring out that it wasn’t so bad to eat only plants and my taste buds started to change, and I started feeling like I had more energy.
So in March of 2015, I made the personal decision and so did my wife to not eat any meat. Since I knew this was the right thing to do but without really preparing for it, I was really hungry for about 2 weeks. I then started figuring out that it wasn’t so bad to eat only plants and my taste buds started to change, and I started feeling like I had more energy.
In the fall of 2015, I was retested in the lab, and I had a 15% increase in my vo2max. And then my power began to improve. This was still no guarantee that I was out of the woods and I continued to read and study to modify my diet and exercise program. The rest, as they say, is history- last year in 2018 I was on the podium at the national championships and missed the podium by one spot at the world championships, and I set an hour record for cycling on a track for an hour at just under 29 miles.
How Does This Apply To You?
So how does this apply to you or somebody you may know that has heart disease? Being an athlete is not unique to having heart disease and having heart disease is not unique to being a non-athlete. So I believe that everything that I experienced applies to the general public.
The caveat of the story is I didn’t just rely on the diet to help me. The link between blood cholesterol and cardiovascular disease is well established in the medical literature. As a matter of fact, it is as closely linked as bacteria is to infection or smoking is to cancer. I’ll get into this a little bit later in some of my lectures, but there is no doubt that even though I had what was considered normal range cholesterol, this had led to the problem because I lived a healthy lifestyle and I thought I had eaten well.
Astounding Results
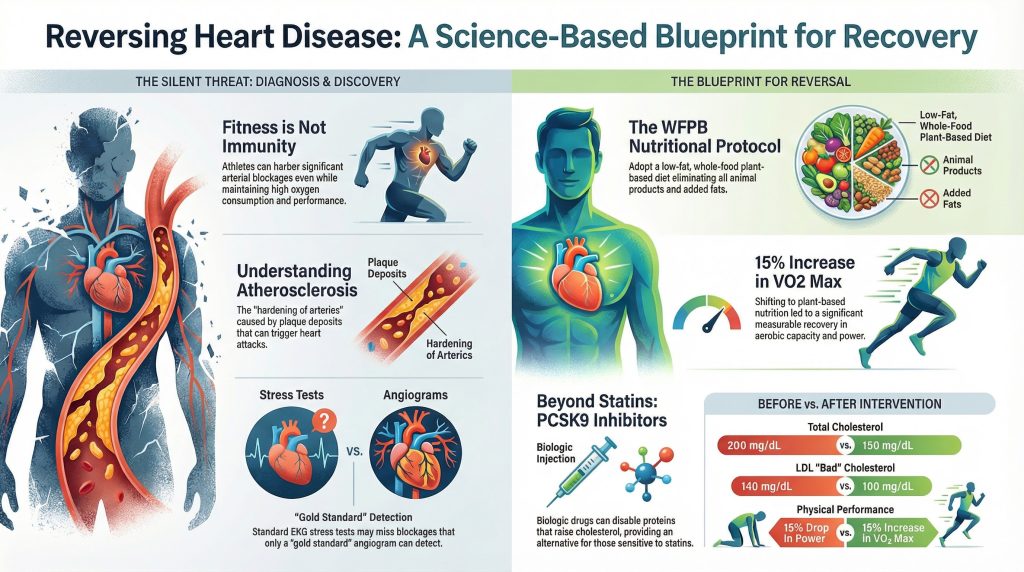
So, soon after changing my diet, my total cholesterol went from about 200 to 150 and my LDL went from about 140 to 100. That was a significant drop, but I also decided to get on medications. I started with statins, but they made my muscles hurt and decreased my performance on the bike, so I petitioned to get on Repatha, also known as Evolocumab, which is a pcsk9 inhibitor. This particular drug is called a biologic and disables a protein that causes your cholesterol to go up, so when you disable this protein your liver can remove more cholesterol from your blood. It operates in a completely different way than statins. The side effect profile according to the literature is near zero. I, in fact, have no side effects from the drug.
At about the same time I decided to start up a support group in my home for other athletes or pretty much anybody who is interested in changing their diet and improving their cardiovascular health. I’ve been running the group now for about 3 years. In the group, we discuss our diet and we have a potluck dinner with low-fat whole foods, and I give a short lecture on scientific topics that the group has asked me to address.
Helping Others Live Rewarding Lives
So it is with this that I will begin an educational series on what I did to improve my health. This informational series is not intended to replace your physician’s guidance or treatment. I am not a physician. I’m going to present the scientific literature and discuss things that I have done to benefit me. Any suggestions that you might get from any of my presentations need to be addressed with your personal health care provider. In other words, talk to your physician first before you do anything that might affect your health.
Some Key Takeaways
A physician is a medical doctor who is trained to treat disease, whereas a Ph.D. is a person who goes through a higher degree to learn a specific topic, do research and write a dissertation which may or not be medically or scientifically oriented.
When I speak of cardiovascular disease, I’m specifically talking about atherosclerosis. Atherosclerosis is also known as hardening of the arteries. It is where the plaque is deposited in the wall of an artery. This plaque can break off and cause a heart attack which can either kill a person or damage part of the heart.
Ultimately my goal is to educate by presenting unbiased scientific information through the lens of my personal experience as a heart disease survivor. Both of my parents and my younger brother, who was only 42 years old, died from heart attacks. My two surviving siblings both have diabetes, and my older brother has cardiovascular disease that we know to be severe. Everything I’ve done has been to save my own life. I didn’t go through medical school to become a cardiologist and treat people with cardiovascular disease, but I also feel that you shouldn’t have to get a Ph.D. and go through what I went through to learn what I did.


